Refugee camps and Covid-19: A crisis within a crisis
September 2021: In the third part of CRJ’s blog series discussing the ongoing Rohingya refugee crisis in Bangladesh, Dr Kazi Sakib outlines how Covid-19 has affected people in the camps, and he looks at the co-ordinated response by humanitarian and government agencies
 The first round of Covid-19 vaccinations was concluded on August 23 in the Rohingya camps, targeting people aged 55 years and above; this equates to 86 per cent coverage. All photos courtesy of the author
The first round of Covid-19 vaccinations was concluded on August 23 in the Rohingya camps, targeting people aged 55 years and above; this equates to 86 per cent coverage. All photos courtesy of the author
Following the mass movement of the Rohingya people from Myanmar on August 25, 2017, many sought shelter in and around the refugee settlements of Kutupalong and Nayapara in Bangladesh’s Cox’s Bazar district. Three years later, the unfolding Covid-19 pandemic exacerbated the pre-existing challenges of congested shelter arrangements and poor water, sanitation and hygiene (WASH) standards.
Currently, more than 889,000 Rohingya people reside in the world’s largest, most densely populated refugee camps. They have a population density of 40,000 people per square kilometre, so the risk of Covid-19 infection is extremely high. The risk of morbidity and mortality is compounded by a nexus of factors, including local transmission (within Bangladesh), limited access to health infrastructure, crowded living settlements, poor health-seeking behaviours, shared sanitary facilities and unhygienic living conditions.
In early April 2020, the first cases of Covid-19 were reported in the local community, followed by the first case in the camps on May 14. Initial projections suggested that at the peak phase there might be thousands of cases per day in the camps. However, despite the range of factors that could have resulted in a catastrophe, these projections were not reached and rates remain low.
As of August 26, 2021, a total of 1,179,827 cases in Bangladesh had been reported. Cases in the local community totalled 12,055, with 2,778 confirmed cases and 30 deaths in the Rohingya camps reported.
With the support of UN agencies and NGOs, and under the guidance of the Ministry of Health and Family Welfare, the Health Sector worked to mitigate the effects of the pandemic among both the Bangladeshi and Rohingya communities by developing and implementing an elaborate Covid-19 response plan.
The Community Health Working Group (CHWG), a subgroup under the health sector, co-ordinates the community health outreach programme in the camps. It takes a community-based approach, with strategic preparedness and response objectives aimed at: Scaling up preventive measures to limit the spread of the disease; establishing community-based surveillance for early identification of active cases, contact tracing and to trigger early warning signs; strengthening health systems to ensure access to health services to save lives and for effective case management; and making vaccines available.
Preventive measures
The Health and WASH sector continues to support preventive interventions, including the promotion of good hygiene and sanitation, as one of the key pillars of the Covid-19 response. Handwashing tippy taps (innovative hands-free devices for handwashing) have been installed in households. The distribution of bath and laundry soap for the refugees, the disinfection of health and WASH facilities, including latrines, water collection points and bathing cubicles are all ongoing.
 Small group sessions, household visits and audio-video messages are just some of the ways that volunteers raise awareness about the need for good hygiene practices in the camps
Small group sessions, household visits and audio-video messages are just some of the ways that volunteers raise awareness about the need for good hygiene practices in the camps
Multi-sectoral volunteers continue to provide information on good hygiene practices, infection prevention protocols, social distancing, the use of face masks and the importance of testing, isolation and quarantine during their household visits. Their messages are disseminated through interpersonal communication and small group sessions using flip charts, leaflets, audio-video messages, as well as various information, education and communication materials.
Community-based surveillance
More than 1,400 community health workers (CHWs) have been deployed to visit refugee households on a weekly basis (on average, each household has four visits per month) to identify individuals suffering with mild respiratory symptoms or moderate/severe Covid-like symptoms.
The CHWs ensure the timely referral of symptom-positive cases to the nearest health facility for testing and, if anyone tests positive, referral is then made to a designated isolation facility, and contacts are referred to quarantine facilities. The CHW will provide information on how to maintain infection prevention measures in the household, measures for patient and care providers, etc. R
egular follow ups are made to ensure that if anyone else in the household develops danger signs, they are referred to the health facility in the quickest possible time.
The community-based surveillance and referral mechanism helped a great deal in the early detection and management of cases, including controlling the potential spread and generating an early alert.
Strengthening healthcare capacity
Since April 2021, a significant increase in the number of Covid-19 positive cases has been reported in the camps. This has also been observed nationally.
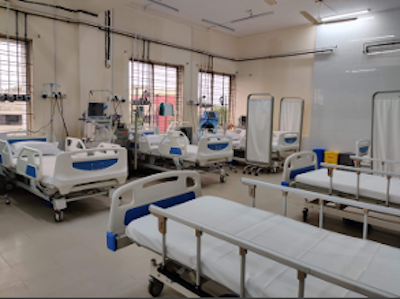
Since the onset of the pandemic, the humanitarian community has ensured better preparedness and response in the camps and surrounding communities, under the leadership of the Government of Bangladesh.
UNHCR – the UN Refugee Agency – helped to establish the first ever intensive care unit (ICU) and High Dependency Unit (HDU) at the Cox’s Bazar Sadar Hospital, with a capacity of ten ICU beds with ventilators, 15 high dependency beds and 13 severe care unit beds. The image to the right shows the ICU in District Hospital, Cox’s Bazar.
To provide care for the severe cases, 13 Covid-19 treatment facilities (SARI ITCs) have been established in the camps and surrounding areas, for both refugee and Bangladeshi patients. The first SARI ITC opened in Ukhiya in May, 2020. With the rapid establishment of the treatment facilities, care was assured to help people get to back to normal life quickly and many lives have been saved as well. Existing capacity is within the levels necessary to respond to an increase in cases: there are currently over 900 beds and approximately 70 per cent are functional, while the remainder can be quickly activated if required.
In terms of testing, there are currently 42 sentinel sites in the camps for the collection of samples. The humanitarian community is looking at scaling up this number to increase access and utilisation by refugees. The Covid-19 testing laboratory in Cox’s Bazar also has an overall capacity to test approximately 1,500 samples per day. The government has also introduced antigen tests to expand access to testing.
A camp-wide contact tracing network has been embedded in the rapid investigation and response teams for Covid-19 to co-ordinate case investigation, contact tracing and isolation. Widespread information sharing and awareness raising campaigns are underway to ensure that the population knows how to reduce the risk of transmitting the virus. IPC (Infection Prevention and Control) training continues, with more than 2,600 humanitarian health workers and government staff trained to date.
Vaccine availability
As part of the national strategy, Bangladesh’s Government included Rohingya refugees living in Bangladesh in both the National Response Plan to Covid-19 as well as the national vaccination plan. The first round of Covid-19 vaccinations was concluded on August 23 in the Rohingya camps, targeting

people aged 55 years and above. A total of 36,943 individuals were vaccinated – this equates to 86 per cent coverage.
The work of multiple-sector volunteers, specifically CHWs, proved to be highly effective in this first round of vaccination. Their role also involved bringing the physically weak or individuals with impairments to the vaccination sites (see right). The CHWs used a strategy that involved integrated advocacy, communication and social mobilisation to reduce vaccine hesitancy with a view to improve vaccine uptake in the camps.
The way forward
As the pandemic has clearly highlighted, no one is safe until everyone is safe. Continued close collaboration between the humanitarian community and the Bangladeshi Government will help to rein in Covid-19, as will continuing with the response activities, including prevention and care in the camps and surrounding local communities.
Covid-19 vaccinations should be extended to ensure full coverage for all refugees above the age of 18, providing the availability and approval from the Government.
Co-ordinated multi-sectoral efforts in the prevention and containment of Covid-19 have already played a vital role and this must be enhanced in the days to come.